Placing Implants in Sites Lacking Keratinized Tissue
A procedure to reconstruct attached gingiva
Timothy F. Kosinski, DDS, MAGD
Implant dentistry has become a predictable and accepted method of replacing missing teeth. Implants can be used to replace one missing tooth or several teeth or to provide support for complete oral rehabilitation in conjunction with permanent or removable implant-retained appliances. When considering treatment options, it is important to determine whether or not a patient is a proper candidate for dental implant therapy. The patient’s medical history must be free of risk factors that are not properly managed. Contraindications to dental implant success include medical conditions such as uncontrolled diabetes, uncontrolled hypertension, or immunosuppressive diseases.
Adequate bone height and width must also be present to support the dental fixture. When adequate bone volume is not available, more invasive bone grafting procedures can be considered. Autogenous bone, or bone taken from another site in the patient’s own mouth, can be harvested and adapted to the defective site. Allograft materials (bone from another human) or alloplastic material (synthetic materials) provide other alternatives. Clinicians should possess a thorough understanding of the oral anatomy in the sites under consideration. Although the position of the mandibular canal, mental foramen, and the maxillary sinus can be demonstrated with digital radiography, the use of cone-beam computed tomography (CBCT) analysis can help clinicians visualize the vital anatomy in the third dimension. Prior to any surgical intervention, computer software can be used to virtually trace the mandibular nerve and place the implants.
Well-engineered implant design has made implant dentistry predictable with positive long-term functional and esthetic results; however, treatment should always begin with a clear visualization of the finished case.
Case Report
A 63-year-old male patient presented to the office with edentulous spaces in the right mandibular arch, requiring dental implant placement and reconstruction of his right second bicuspid and first molar. A review of his medical history revealed controlled hypertension, some peripheral neuropathy, and controlled acid reflux. The patient expressed a desire to have his mandibular arch restored with fixed crown and bridgework. Although a new removable partial denture was proposed as an option, the patient ultimately elected to have dental implants placed.
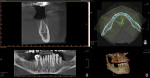
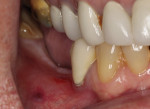
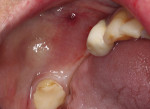
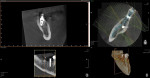
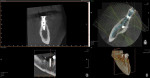
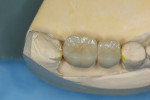
A CBCT scan (PaX-i3D Green, Vatech America Inc.) taken of the edentulous ridge revealed severe vertical bone loss (Figure 1). When teeth are extracted, the bone often resorbs apically and horizontally toward the lingual, making the ridge shorter and narrower. Note the narrow coronal portion of the bone, which can present a challenge when surgically placing implants. This bone loss is sometimes accompanied by mucosal tissue following the bone, resulting in a lack of attached gingiva on the facial/buccal aspect of the edentulous site.1 In this case, the amount of vertical and horizontal bone degeneration created by the loss of the natural teeth is readily apparent (Figure 2 and Figure 3). It should also be noted that the patient’s most posterior molar tooth will eventually require restoration with a conventional crown.
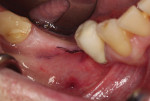
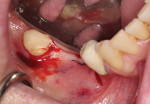
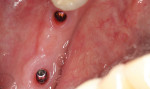
The mucogingival line, drawn in black, demarks the attached gingiva, which is critical to the long-term success of dental implants and the mucosal tissue (Figure 4). Mucosa is flexible and does not provide adequate protection on the buccal aspect of the planned implant site. The absence of attached gingiva can lead to bacterial invagination and, ultimately, peri-implant disease. Attempting to place dental implants without considering the attached gingiva available could result in the presence of mucosal tissue on the buccal aspect of the implants, which can cause discomfort, maintenance problems, and possible bone loss surrounding the site.
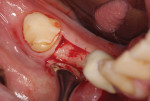
Following the administration of a local anesthetic, an Orban knife (Golden Dental Solutions) was used to make a controlled incision on the lingual aspect of the edentulous ridge where the attached gingiva was adequate and around the adjacent teeth (Figure 5). This was done with the intention of eventually creating a band of attached gingiva 2 mm to 3 mm in width on the buccal aspect, following implant placement. The band of attached gingiva was then moved buccally from the lingual portion of the crest (Figure 6). The lingual tissue was not elevated and remains intact and attached to the underlying bone. In addition, reflecting a full thickness gingival flap provides an opportunity for the availability of underlying bone to be determined.
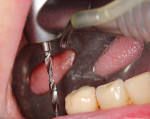
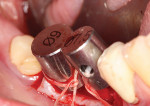
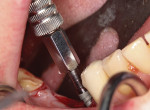
The osteotomy was initiated using a 2.2 mm diameter pilot drill, which is used to penetrate the cortical bone, but not taken to depth (Figure 7). This bur is used to create proper mesial-distal and facial-lingual angulation. To help visualize the eventual emergence profile of the final implant-retained crowns, an MD Guide (Golden Dental Solutions) was employed. These cylinders of five various diameters are used to simulate the mesial-distal width of the natural dentition. The MD Guide enables the drilling of a pilot hole with the desired mesial-distal spacing and parallelism, without altering the current surgical protocol (Figure 8). Should the MD Guide require repositioning, the minimal hole created by the pilot drill will not hamper final site development.
After idealizing the angulation and depth using the pilot drill, osteotomy burs of various diameters were used to create the final opening in the bone for the dental implants (Figure 9). Note that the osteotomy burs should create a site slightly smaller than the final diameter of each implant. The Hahn™ Tapered Implant System (Glidewell) was chosen because the tapered body of the implant features prominent threads, which helps ease placement into an undersized osteotomy (Figure 10). These implants are engineered to facilitate precise angulation and positioning during placement. The buttress thread pattern provides good initial stability and minimizes resorption in all bone types, while the coronal microthreads aid in the preservation of crestal bone. To promote osseointegration, the surface of the implant is treated with resorbable blast media.2,3 In addition, its machined collar facilitates soft tissue maintenance, and its conical, internal hex connection provides a secure, stable prosthetic seal.
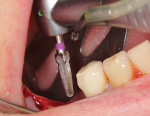
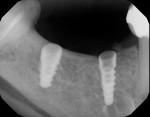
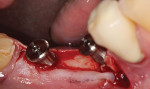
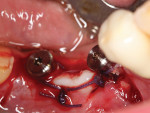
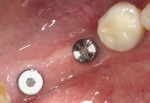
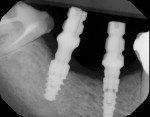
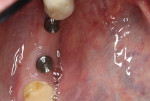
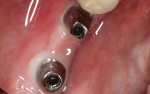
Prior to placement, the apex of the adjacent tooth was used as a guide to determine the appropriate depth away from the mandibular canal. Because the tissue at the site was simply infiltrated with anesthesia, and no mandibular block was performed, the patient’s sensations could help the practitioner determine the implant’s proximity to the nerve during placement. A Ø 3.5 x 10 mm Hahn dental implant was placed into the surgical site of the mandibular right second bicuspid and torqued to 40 Ncm to achieve initial stability (Figure 11 and Figure 12). Next, a Ø 4.3 x 8 mm Hahn implant was placed in the site of the mandibular first molar and also torqued to 40 Ncm. A radiograph was taken to ensure ideal placement of the implants at the crest of the available bone (Figure 13). Because both implants were torqued to greater than 35 Ncm, 5 mm tall healing abutments were threaded into the implants and torqued to 25 Ncm to provide a point for re-attachment and formation of the gingiva (Figure 14 and Figure 15).4
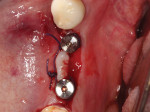
After placing the healing abutments, the band of attached gingiva taken from the lingual aspect of the ridge was then repositioned and adapted to the buccal aspect of the healing abutments. The lingual tissue was not engaged. VICRYL sutures (Ethicon) were used to suture the tissue around the healing abutments (Figure 16), and the 2 mm to 3 mm open wound on the lingual aspect of the surgical site was left uncovered and allowed to regenerate on its own (Figure 17). A postoperative CBCT scan was taken, which illustrates the ideal positioning of the dental implants in the bicuspid and molar regions (Figure 18 and Figure 19). After 7 days, the sutures were removed.
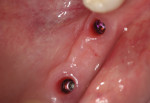
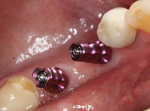
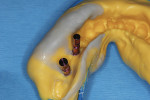
The implants were allowed to integrate for approximately 4 months, at which time the patient was recalled to the office to evaluate the tissue health and make a final impression of the internal design of the implants. Upon examination, the gingival tissue around the healing abutments demonstrated a lack of inflammation, and the incision gap left at surgery was filled and covered with attached keratinized gingiva (Figure 20). Once the healing abutments were removed, it could be seen that a healthy tissue cuff had formed around them with a band of attached gingiva on the buccal aspect of the edentulous site (Figure 21). In addition, the mucogingival line had been moved down the vestibule significantly. Impression copings were placed to engage the inside components of the implants (Figure 22), and a digital radiograph was taken to ensure that the metal components were completely seated (Figure 23). The impression was captured with conventional impression techniques using medium and heavy body Panasil vinyl polysiloxane material (Kettenbach). Then, the implant transfer assemblies were threaded into the lab analogues and inserted into the final impression (Figure 24 and Figure 25).
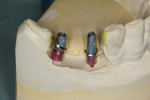
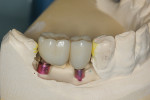
The final impressions were sent to the Glidewell dental laboratory, where custom titanium abutments were created using innovative CAD/CAM design. At the lab, a master cast was created; custom abutments, which engage the internal design of the implants, were prepared; and individual Bruxzir zirconia crowns were fabricated to exhibit proper emergence (Figure 26 and Figure 27).
After the crowns were delivered, the healing abutments were again removed, revealing healthy pink gingiva around the implants (Figure 28 and Figure 29). The prepared abutments were then inserted into the implants and torqued to 35 Ncm (Figure 30). The margins of the abutments are at the gingival contour, thus preventing subgingival margins and the potential for periodontal problems resulting from excess cement being pushed subgingivally. The abutments were torqued to 35 Ncm using a torque wrench, and the Bruxzir zirconia crowns were cemented with Improv® Temporary Implant Cement (Alvelogro) (Figure 31). The use of a “soft” cement when seating implant-retained crowns ensures that if any issues arise with the crown or the implant itself, the crown can be removed to allow access to the abutment or the body of the implant.
Conclusion
Healthy gingival margins are critical to the long-term success of dental implants. The attached gingiva offers protection from external injury and is vital to proper tissue healing around dental implants. Without the attached keratinized gingiva, food impaction may occur as well as bacterial penetration and tissue shrinkage—all of which may affect the long-term prognosis and esthetics of implants. In addition, keratinized tissue is critical in areas of the mouth where plaque control may be compromised. Hemidesmosomal fibers attach the junctional epithelium to the teeth or implants, and the oral sulcular epithelium is connected to the junctional epithelium.5 Therefore, the gingiva around dental implants needs to be firm and attached, otherwise the physiologic pattern of health may be broken. Subjacent to the junctional epithelium is a connective tissue layer about 1 mm thick. Unlike in teeth, where the connective tissue fibers are perpendicular to the root surfaces and insert into the cementum, around implants, the connective tissue fibers are parallel or oblique and do not insert into the implant surface. Because there is no periodontal ligament around implants, there is less blood supply than there is around teeth.6 Following tooth loss, mucosal tissue often migrates at or near the crest of the edentulous ridge.
Simple surgical procedures can be performed to properly position the attached gingiva on the buccal/facial aspect of dental implants. Selecting the most appropriate surgical technique is accomplished by understanding the vital anatomy, utilizing proper diagnostic tools, evaluating tissue restraints, and considering all of the restorative options available. Creating crowns that emerge from the tissue provides an outstanding tooth replacement solution for patients, restoring function and maximizing oral hygiene.
References
1. Carnio J, Camargo PM, Passaezi E. Increasing the apico-coronal dimension of attached gingiva using the modified apically repositioned flap technique: a case series with 6 month follow up. J Periodontol. 2007;78(9):1825-1830.
2. Piattelli M, Scarano A, Paolantonio M, Iezzi G, Petrone G, Piatelli A. Bone response to machined and resorbable blast material titanium implants: an experimental study in rabbits. J Oral Implantol. 2002:28(1)2-8.
3. Nishimoto SK, Nishimoto M, Park SW, et al. The effect of titanium surface roughening on protein absorption, cell attachment and cell spreading. Int J Oral Maxillofac Implants. 2008;23(4):675-680.
4. Degidi M. Daprile G, Piattelli A. Influence of underpreparation on primary stability of implants inserted in poor quality bone sites: an in vitro study. J Oral Maxillofacial Surg. 2015;73(6):1084-1088.
5. Lang NP, Löe H. The relationship between the width of keratinized gingiva and gingival health. J Periodontol. 1972;43(10):623-627.
6. Beagle JR. Developing keratinized mucosa around nonsubmerged dental implants. Part II: The use of non vascularized soft tissue grafts. Periodontal Practice Today. 2005;2(4):259-266.
About the Author
Timothy F. Kosinski, DDS, MAGD
Private Practice
Bingham Farms, Michigan